What are treatments for frozen shoulder
Frozen shoulder can be left untreated, but the pain and stiffness may persist for up to three years. Recovery can be significantly improved with one or more of the following courses of treatment:
- Physiotherapy
- Medication
- Surgery
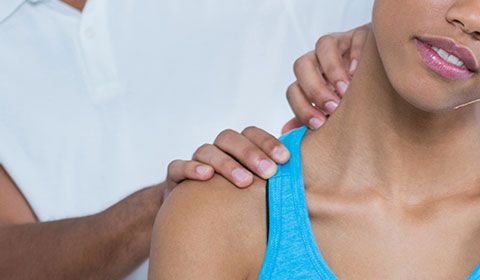
Physiotherapy
The most common, and often most successful treatment for frozen shoulder is physiotherapy. A trained physiotherapist will focus on stretching the shoulder joint to improve mobility and relieve pressure on the joint. Therapy can take anywhere from a few weeks to nine months depending on age, severity and other contributing conditions. A physiotherapist may also recommend self-directed gentle range of motion exercises that can be performed at home.
Medications
If severe pain and/or stiffness is inhibiting quality of life and physiotherapy alone is not alleviating the condition, there are a number of medications that can help relieve the symptoms of frozen shoulder. Prescriptions can be as mild as anti-inflammatory medication such as aspirin, ibuprofen, or naproxen sodium, through to more significant treatments such as steroid injections directly into the shoulder joint.
Surgery
If physiotherapy does not improve the frozen shoulder symptoms, a doctor may recommend surgery.
Surgery can range in complexity and invasiveness depending on the severity of scar tissue buildup.
In cases where the buildup is mild but painful, a surgeon can simply manipulate the shoulder through a full range of motion under a general anesthetic to help break up any adhesions.
In cases where there is significant scar tissue buildup, a surgeon may conduct arthroscopic surgery, which involves making a small cut in the shoulder and using a camera to remove scar tissue manually.
Most forms of frozen shoulder surgery are performed on an outpatient basis. Post-operative physiotherapy is typically still required. Most patients will have their full range of motion back within three months.